AbstractMany chronic insomnia patients use sleep medication well beyond the recommended duration, and patients who are hypnotic-dependent encounter several challenges when attempting to discontinue. The current article presents these challenges and reviews studies that have added cognitive-behavioral therapy for insomnia (CBTI) to a gradual tapering program to facilitate discontinuation of hypnotic medication in chronic insomnia patients. The current literature provides substantial support for using CBTI to facilitate discontinuation of hypnotic medication in chronic insomnia patients. Across several randomized clinical trials, the majority of the findings indicate that using CBTI, delivered by a therapist or self-help, along with a supervised or gradual tapering program is superior to tapering only or CBTI only in terms of medication discontinuation. Although these results are promising, it should be noted that the long-term evidence is more equivocal, as over 40% of patients relapse in the need for sleep medication within 2 years, which may highlight the importance of adding follow-up booster sessions in hypnotic-dependent insomniacs. These findings indicate that rather than choosing between CBT and hypnotic medication, clinicians might be better served using both treatment modalities to optimize the relative strengths of each treatment. Such an approach represents a more modern view of treating chronic insomnia patients by using both pharmacological and non-pharmacological tools.
INTRODUCTIONInsomnia is a highly prevalent disorder that affects 10–15% of the general population.1,2 Chronic insomnia is associated with significant morbidity, such as reduced quality of life, increased risk for psychiatric disorder, and higher risk for various physical diseases such as hypertension and diabetes.1,3–7 Over the past 20 to 30 years, several clinical trials have examined the efficacy of various treatments for insomnia. The accumulated research evidence supports the efficacy of both pharmacological and non-pharmacological treatments for insomnia, yet each of these treatment modalities has limitations in clinical practice. A sophisticated approach that has gained research attention and appears to be translatable to real-world clinical practice is to combine a pharmacological treatment with a non-pharmacological treatment. Specifically, cognitive-behavior therapy for insomnia (CBTI) has been used to aid in the discontinuation of chronic hypnotic use among those who began using hypnotics and have become chronic users. The aims of this paper are to present the issues related to chronic hypnotic use and to review the literature on the addition of CBTI to facilitate the discontinuation of hypnotic medication in chronic insomnia patients.
Pharmacological Treatment of Insomnia: Hypnotic MedicationHistorically, pharmacotherapy has been the first line treatment for insomnia and remains a popular choice of treatment.8,9 Approximately 3 to 10% of the general population use hypnotic medication, and this rate increases to 20% among older individuals.10–13 Overall, studies have demonstrated that hypnotics can improve sleep by reducing sleep onset latency and increasing total sleep time and these effects occur within the first week of initiating treatment.14–16 Currently, the most commonly used medications for insomnia include benzodiazepine receptor agonists (BzRAs), melatonin receptor agonists, and antidepressants.17 There are now 10 medications approved by the Food and Drug Administration to treat insomnia (Table 1) and the recommended use is between 30 and 180 days. However, about 65% of individuals who are prescribed sleep medication continue to use them for more than one year, with a substantial number of individuals continuing to use sleep medications for more than 5 years.18–20 These patterns of long-term use hypnotic use are particularly common in primary care settings. Long-term hypnotic use has raised concerns given findings of psychomotor and cognitive impairment, difficulties with discontinuation, and dependence liability that are associated with prolonged use.21 In older adults, there may be concerns about falls and hip fractures, motor vehicle accidents, and mortality, as well as concerns for undesirable drug interactions and polypharmacy effects.22–24 Despite the rapid onset of treatment effects, a major concern with the treatment of insomnia using hypnotic medication is the difficulty of preventing long-term dependency.
A Pattern of Hypnotic DependencyChronic insomnia patients who are hypnotic-dependent encounter several challenges when attempting to discontinue (Fig. 1). First, many chronic hypnotic users develop tolerance towards the medication, and need to increase dosages or switch to more potent sleep medication if the initial dose is no longer sufficient for promoting sleep. This might lead to greater risk of adverse side effects or even overdose from the medication. As tolerance increases, some patients might develop a physical or psychological dependence on the drug. Physical dependence involves a reliance on the drug to sleep or else withdrawal symptoms occur. The most frequently observed symptom, rebound insomnia, is characterized by a brief worsening of insomnia symptoms (1 to 2 nights) beyond baseline immediately after discontinuing hypnotic medication. Studies have shown that rebound insomnia is likely to occur after using high doses of BzRAs that are short or intermediate acting, but less likely with long acting drugs.25 Thus, when discontinuing BzRAs, a gradual tapering of the dose over a few nights is recommended to avoid rebound insomnia.25 It has been suggested that experiencing rebound insomnia may motivate insomnia patients to continue chronic use of sleep hypnotics long-term. Schneider-Helmert26 suggested that rebound insomnia in association with an overestimation of the efficacy of sleep medication may lead to continued chronic use of the medication, increased tolerance of the hypnotic that leads to taking higher doses of medication, and eventually developing dependence towards the medication. In addition to physical dependence, many patients develop psychological dependence, or a fear that sleep will be worse without medication.27 Many insomnia patients may try to discontinue sleep medication on their own, but experience rebound insomnia which perpetuates the fear of not using sleep medication, thus leading to a pattern of chronic hypnotic use. Fig. 1 depicts a typical pattern of chronic hypnotic dependency.
Non-Pharmacological Treatment of Insomnia: Cognitive-Behavioral Therapy for Insomnia (CBTI)CBTI is a short-term treatment that is based on cognitive and behavioral principles to treat insomnia. The main purpose of CBTI is to eliminate maintaining factors that are presumed to perpetuate chronic insomnia. CBTI usually consists of 4–8 sessions and utilizes a multicomponent approach that includes sleep hygiene, sleep restriction, stimulus control, relaxation training, and cognitive therapy.28 Table 2 describes these components in detail. CBTI has become the “gold standard” for non-pharmacological treatment for chronic insomnia based on strong empirical evidence.29,30 There have been over 30 treatment studies that have examined the effectiveness of CBTI as a treatment for insomnia, which have been summarized and reviewed by a commissioned task force in 2006 and several meta-analyses. CBTI has been shown to produce long-term improvements in sleep quality among 70–80% of insomnia patients, and has been known to be preferred over pharmacotherapy.31–34 CBTI also leads to reliable improvements in nocturnal symptoms of insomnia, including reduced sleep latency, reduced number and duration of awakenings, increased total sleep time, and improved sleep quality. Moreover, CBTI has been recommended for the treatment of both primary and secondary insomnia.30 Despite the strong evidence for efficacy, CBTI is time- intensive for the patient and there are currently an insufficient number of trained clinicians to handle the high prevalence of insomnia. In addition, the improvements in sleep do not usually occur as rapidly in CBTI as those seen in hypnotics, where sleep improvements typically occur within the first week.
Review of Studies Combining CBTI with Sleep Medication DiscontinuationIn addition to CBTI as a primary treatment, the AASM practice parameters also recommend the use of CBTI in treating insomnia patients who were chronic hypnotic users.30 Given the potential risk of long-term hypnotic use, clinicians are often met with the challenge of how to help their patients discontinue hypnotic medication while managing their insomnia. One novel approach has been to combine a non-pharmacological treatment, such as CBTI, to aid in the discontinuation of sleep medication in chronic insomnia patients. There have been several uncontrolled studies or small clinical trials (n < 30), and two large scale randomized clinical trials that have investigated utilizing CBTI to facilitate discontinuation of hypnotic medication.
One of the first studies in this area was conducted by Morin et al.,35 who used CBTI combined with a supervised medication tapering schedule in a multiple baseline design with 5 insomnia patients who were dependent on benzodiazepines (alprazolam, diazepam, lorazepam) at least 4 nights per week (range of duration for benzodiazepine use = 2–15 years). Among the 5 participants, 4 were successful in discontinuing medication within 6–8 weeks, and 3 patients remained drug-free at 3-month follow-up. While sleep efficiency decreased from baseline to the end of the medication withdrawal phase, sleep efficiency improved at 3-month follow-up. This seminal study demonstrated the potential effects of combining CBTI with a medication tapering program, but the sample size and methodological rigor was very limited.
Riedel et al.36 examined 21 medicated and 20 non-medicated individuals with insomnia who were participating in a sleep medication withdrawal program that provided psychoeducation about a gradual tapering system. The medicated insomniacs were using sleep medication at least 6 times per week for at least 3 weeks (mean duration 4.7 years). Sleep medications included benzodiazepines (alprazolam, lorazepam, temazepam, triazolam, chloraepate, clonazepam, estazolam, quazepam) and/or antidepressants (amitriptyline, doxepin, trazodone, imipramine) as well as over-the-counter medication. Half of the participants in the sleep medication group and half of the participants in the nonmedication group received stimulus control treatment in addition to the withdrawal program. Medication consumption was defined in two ways - frequency of medication taken during the phase of the study, and percent reduction of medication dosage from baseline to posttreatment, and posttreatment to follow-up. Results from their study indicated that participants were using sleep medication an average of 6.2 nights per week at baseline, which reduced significantly to 1.7 nights per week through a gradual withdrawal program, and participants reduced their medication dosage by 76.6% without experiencing aversive sleep deterioration. However, at follow-up, some relapse was reported as medicated participants increased their frequency of sleep medication use to 3.1 nights per week, with increases in dosages. Although stimulus control treatment did not improve patient’s ability to reduce sleep medication, adding a stimulus control treatment to a gradual tapering program improved sleep and daytime functioning after medication reduction, compared to those who did not receive stimulus control treatment. Additionally, this study also showed the difficulty of sustaining treatment effects long-term, which indicates the importance of having follow-up booster sessions to continue treatment effects.
In testing another component of CBTI, Lichstein et al.37 explored the effectiveness of adding relaxation to assist in sleep medication withdrawal. Forty participants (only half using chronic sleep medication) participated in the study, and half of the medicated participants and unmedicated participants received progressive muscle relaxation. The medicated participants were taking benzodiazepines, antidepressants, and over-the-counter medication (mean duration = 5.9 years). All medicated participants received a gradual sleep medication tapering program, and sleep medication consumption reduced by nearly 80% at post-treatment. Participants who received relaxation therapy in addition to the tapering program obtained additional benefits in sleep efficiency, sleep quality, and reduced withdrawal symptoms. Relaxation therapy benefited both medicated and nonmedicated participants, and the authors concluded that adding relaxation therapy in addition to a medication tapering program may be beneficial for hypnotic-dependent insomniacs.
Using improved methodology, two randomized clinical trials have investigated the effectiveness of CBTI in the context of hypnotic discontinuation. First, a study by Morin et al.38 conducted a randomized clinical trial comparing a supervised tapering program, CBTI, or combined treatment (supervised tapering with CBTI) on 76 individuals with long-term benzodiazepine use (mean duration 19.3 years). While all three interventions significantly helped reduce both the quantity and frequency of benzodiazepine use after the 10-week intervention period, individuals who received a combination of both supervised tapering and CBTI had significantly higher proportion of individuals who remained benzodiazepine-free at post-treatment (85%) compared to those who received a medication taper alone (48%) or CBTI alone (54%). Individuals who received both CBTI and medication tapering, or CBTI alone had greater subjective sleep improvements compared to individuals who received a medication taper alone. This study provided more definitive evidence that the combination of CBTI with a structured tapering program is needed to obtain the optimal outcome for hypnotic discontinuation.
In addition to the acute effects, In addition to the acute effects, Morin et al.41 also examined the long-term effects and relapse rates of individuals from the study above38. While there was a high rate of relapse for sleep medication across all three conditions (42.6%), participants who either received a supervised medication taper (30.8%) or combined approach (33.3%) had significantly less relapse rates compared to the CBTI only group (69.2%). Additionally, time to relapse was significantly longer for both the medication taper only group (18.6 months) and combined treatment (12.6 months) compared to the CBTI only group (8.5 months). Similar to the earlier findings of Riedel and colleagues (1998), the short-term benefits of these interventions are somewhat diminished by the high relapse rates and suggest that CBTI booster sessions may be useful in preventing relapse of hypnotic use.
Another randomized clinical trial by Belleville et al.10 extended the Morin et al.38 study by testing a self-help CBTI program to see if it a more conservative method of CBTI that uses fewer resources could also produce similar results. In this study, an 8-week hypnotic taper program alone was compared with the tapering program combined with a self-help CBTI program in 53 chronic users of hypnotics (benzodiazepines, zopliclone, zaleplon) whose average use of sleep medication was 6.75 nights per week (mean duration = 14.1 years). Both groups decreased frequency (less than once a week) of hypnotic use, and nightly dosage (lorazepam equivalent) decreased from 1.67 mg to 0.12 mg. Individuals who received CBTI combined with the tapering program showed improvements in sleep efficiency and total wake time, compared to those who received a tapering program alone. These findings suggest that the addition of a self-help CBTI to a tapering program over 8 weeks could be an alternative and cost-effective option for individuals who might not have access to a CBTI therapist.
In addition to the promising outcome evidence indicating that the addition of CBTI to a gradual tapering program leads to improvements in insomnia symptoms as well as reductions in the frequency and dosage of medication, another group of studies have examined baseline symptomotology and psychological factors that can predict successful medication discontinuation. Belanger et al.39 conducted secondary analyses from the Morin et al.38 dataset and found that compliance with treatment and success in reducing hypnotic medication was significantly associated with self-efficacy. Belleville and Morin40 also conducted secondary analyses of the Belleville et al.10 study comparing a hypnotic taper program with or without self-help CBTI. They reported that while there were no significant psychological differences at baseline between medication-free individuals and those still using medication at the end of a taper intervention, group differences emerged midway during treatment. Participants who remained medication-free at 6-month follow-up had less severe insomnia and anxiety symptoms, more positive perceived health and higher self-efficacy about refraining from using hypnotics at 6-month follow-up. Together, these findings suggest that severity of insomnia, self-efficacy, and perception of health are important factors to evaluate in determining candidates who may need more intensive and individualized therapeutic attention to target these factors, which would subsequently lead to higher likelihood in benefitting from using CBTI as part of a medication tapering program.
Finally, a recent study by Morin et al.41 examined different sequential pathways of CBTI only, and CBTI plus zolpidem. The aim of this study was not specifically on medication tapering, but rather to test different sequences of initiating and tapering pharmacological and non-pharmacological treatments. In terms of short-term outcomes at 6 weeks, the rates of remission and response for CBTI only was found to be similar to CBTI plus zolpidem. However, in terms of long-term outcomes at 6 months, the combined treatment was superior to CBTI alone, with the best outcome achieved by using CBT plus zolpidem for the first 6 weeks, followed by CBTI alone during the maintenance phase. A key strength of this study is that the treatment sequences are similar to real-world decisions made in the clinic and thus can be more readily implemented into clinical practice.
CONCLUSIONBased on the literature reviewed, there appears to be substantial support for using CBTI to facilitate discontinuation of hypnotic medication in chronic insomnia patients. Across several randomized clinical trials, the majority of the findings indicate that using CBTI, delivered by a therapist or self-help, along with a supervised or gradual tapering program is superior to tapering only or CBTI only in terms of medication discontinuation and insomnia symptoms. The findings also indicate that patients who have more severe insomnia, a more negative perception of health, and lower self-efficacy after treatment are more likely to have difficulty in discontinuing hypnotics compared to patients who do not exhibit these characteristics after receiving treatment. This indicates that these individuals may need more intensive and individualized therapeutic attention following treatment to benefit from receiving CBTI in addition to a medication tapering program. Although these results are promising, it should be noted that the long-term evidence is more equivocal, as over 40% of patients relapse in the need for sleep medication within 2 years, which may highlight the importance of adding follow-up booster sessions in hypnotic-dependent insomniacs.
These findings have important implications for optimizing patient care in the sleep clinic. Rather than choosing between CBT and hypnotic medication, clinicians might be better served using both treatment modalities to optimize the relative strengths of each treatment. Since the benefits of hypnotic medication occurs rapidly, within the first week, and CBTI has demonstrated long-term effects, a combination of the two approaches might yield both immediate and long-term relief from insomnia. Such an approach represents a more modern view of treating chronic insomnia patients by systematically using both pharmacological and non-pharmacological tools. It is hoped that further research and training of sleep clinicians will encourage the use of multidisciplinary teams that can integrate these treatments rather than choosing between the treatments in a limited clinical practice.
REFERENCES1. Ford DE, Kamerow DB. Epidemiologic study of sleep disturbances and psychiatric disorders. An opportunity for prevention? JAMA 1989;262:1479-84.
2. Ohayon MM. Epidemiology of insomnia: what we know and what we still need to learn. Sleep Med Rev 2002;6:97-111.
3. Buysse DJ, Reynolds CF 3rd, Kupfer DJ, Thorpy MJ, Bixler E, Manfredi R, et al. Clinical diagnoses in 216 insomnia patients using the International Classification of Sleep Disorders (ICSD), DSM-IV and ICD-10 categories: a report from the APA/NIMH DSM-IV Field Trial. Sleep 1994;17:630-7.
4. Dodge R, Cline MG, Quan SF. The natural history of insomnia and its relationship to respiratory symptoms. Arch Intern Med 1995;155:1797-800.
5. Foley D, Ancoli-Israel S, Britz P, Walsh J. Sleep disturbances and chronic disease in older adults: results of the 2003 National Sleep Foundation Sleep in America Survey. J Psychosom Res 2004;56:497-502.
6. Foley DJ, Monjan AA, Brown SL, Simonsick EM, Wallace RB, Blazer DG. Sleep complaints among elderly persons: an epidemiologic study of three communities. Sleep 1995;18:425-32.
7. Katz DA, McHorney CA. Clinical correlates of insomnia in patients with chronic illness. Arch Intern Med 1998;158:1099-107.
8. Ohayon MM, Caulet M, Priest RG, Guilleminault C. Psychotropic medication consumption patterns in the UK general population. J Clin Epidemiol 1998;51:273-83.
9. Simon GE, VonKorff M. Prevalence, burden, and treatment of insomnia in primary care. Am J Psychiatry 1997;154:1417-23.
10. Belleville G, Guay C, Guay B, Morin CM. Hypnotic taper with or without self-help treatment of insomnia: a randomized clinical trial. J Consult Clin Psychol 2007;75:325-35.
11. Hohagen F, Käppler C, Schramm E, Rink K, Weyerer S, Riemann D, et al. Prevalence of insomnia in elderly general practice attenders and the current treatment modalities. Acta Psychiatr Scand 1994;90:102-8.
12. Mellinger GD, Balter MB, Uhlenhuth EH. Insomnia and its treatment. Prevalence and correlates. Arch Gen Psychiatry 1985;42:225-32.
13. Ohayon MM, Caulet M. Psychotropic medication and insomnia complaints in two epidemiological studies. Can J Psychiatry 1996;41:457-64.
14. Holbrook AM, Crowther R, Lotter A, Cheng C, King D. Meta-analysis of benzodiazepine use in the treatment of insomnia. CMAJ 2000;162:225-33.
15. Krystal AD, Walsh JK, Laska E, Caron J, Amato DA, Wessel TC, et al. Sustained efficacy of eszopiclone over 6 months of nightly treatment: results of a randomized, double-blind, placebo-controlled study in adults with chronic insomnia. Sleep 2003;26:793-9.
16. Smith IE, Quinnell TG. Pharmacotherapies for obstructive sleep apnoea: where are we now? Drugs 2004;64:1385-99.
17. Feren S, Schweitzer PK, Walsh JK. Pharmacotherapy for insomnia. Handb Clin Neurol 2011;99:747-62.
18. National Institutes of Health. National Institutes of Health State of the Science Conference statement on Manifestations and Management of Chronic Insomnia in Adults, June 13–15, 2005. Sleep 2005;28:1049-57.
19. Morgan K, Dallosso H, Ebrahim S, Arie T, Fentem PH. Prevalence, frequency, and duration of hypnotic drug use among the elderly living at home. Br Med J (Clin Res Ed) 1988;296:601-2.
20. Morgan K, Fentem PH. Sleep and aging. In Lichstein KL, Morin CM (eds.), Treatment of late-life insomnia. Thousand Oaks, CA: Sage Publications; 2000. pp. 3-36.
21. Roth T, Roehrs T, Vogel G. Zolpidem in the treatment of transient insomnia: a double-blind, randomized comparison with placebo. Sleep 1995;18:246-51.
22. Hemmelgarn B, Suissa S, Huang A, Boivin JF, Pinard G. Benzodiazepine use and the risk of motor vehicle crash in the elderly. JAMA 1997;278:27-31.
23. Kripke DF, Klauber MR, Wingard DL, Fell RL, Assmus JD, Garfinkel L. Mortality hazard associated with prescription hypnotics. Biol Psychiatry 1998;43:687-93.
24. Ray WA, Griffin MR, Schaffner W, Baugh DK, Melton LJ 3rd. Psychotropic drug use and the risk of hip fracture. N Engl J Med 1987;316:363-9.
26. Schneider-Helmert D. Why low-dose benzodiazepine-dependent insomniacs can’t escape their sleeping pills. Acta Psychiatr Scand 1988;78:706-11.
27. Gillin JC, Byerley WF. Drug therapy: The diagnosis and management of insomnia. N Engl J Med 1990;322:239-48.
28. Smith MT, Huang MI, Manber R. Cognitive behavior therapy for chronic insomnia occurring within the context of medical and psychiatric disorders. Clin Psychol Rev 2005;25:559-92.
29. National Institutes of Health. National Institutes of Health State of the Science Conference statement on Manifestations and Management of Chronic Insomnia in Adults, June 13–15, 2005. Sleep 2005;28:1049-57.
30. Morgenthaler T, Kramer M, Alessi C, Friedman L, Boehlecke B, Brown T, et al. Practice parameters for the psychological and behavioral treatment of insomnia: an update. An american academy of sleep medicine report. Sleep 2006;29:1415-9.
31. Morin CM, Colecchi C, Stone J, Sood R, Brink D. Behavioral and pharmacological therapies for late-life insomnia: a randomized controlled trial. JAMA 1999;281:991-9.
32. Morin CM, Culbert JP, Schwartz SM. Nonpharmacological interventions for insomnia: a meta-analysis of treatment efficacy. Am J Psychiatry 1994;151:1172-80.
33. Morin CM, Hauri PJ, Espie CA, Spielman AJ, Buysse DJ, Bootzin RR. Nonpharmacologic treatment of chronic insomnia. An American Academy of Sleep Medicine review. Sleep 1999;22:1134-56.
34. Morin CM, Mimeault V, Gagné A. Nonpharmacological treatment of late-life insomnia. J Psychosom Res 1999;46:103-16.
35. Morin CM, Colecchi CA, Ling WD, Sood RK. Cognitive behavior therapy to facilitate benzodiazepine discontinuation among hypnotic-dependent patients with insomnia. Behav Ther 1995;26:733-45.
36. Riedel B, Lichstein K, Peterson BA, Epperson MT, Means MK, Aguillard RN. A comparison of the efficacy of stimulus control for medicated and nonmedicated insomniacs. Behav Modif 1998;22:3-28.
37. Lichstein KL, Peterson BA, Riedel BW, Means MK, Epperson MT, Aguillard RN. Relaxation to assist sleep medication withdrawal. Behav Modif 1999;23:379-402.
38. Morin CM, Bastien C, Guay B, Radouco-Thomas M, Leblanc J, Vallières A. Randomized clinical trial of supervised tapering and cognitive behavior therapy to facilitate benzodiazepine discontinuation in older adults with chronic insomnia. Am J Psychiatry 2004;161:332-42.
39. Bélanger L, Morin CM, Bastien C, Ladouceur R. Self-efficacy and compliance with benzodiazepine taper in older adults with chronic insomnia. Health Psychol 2005;24:281-7.
Fig. 1.Difficulty of discontinuing hypnotic medication in insomnia patients. From the educational material of “Introduction of Cognitive-Behavioral Therapy for insomnia” by S. Chung, in “Insomnia symposium 2010” held by The Korean Society of Sleep Medicine. 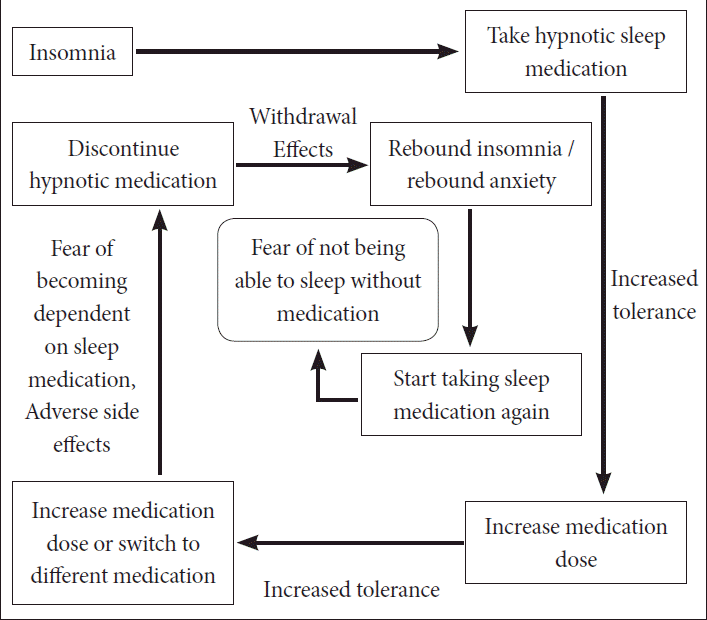
Table 1.Selected drugs used for insomnia in the United States*
These constitute the most commonly used agents for the management of insomnia in the United States, either by prescription or over the counter (OTC). Among those drugs with a Food and Drug Administration (FDA) indication for insomnia, flurazepam, and quazepam are not often used because of their long duration of action and predisposition to residual sedation. Among the drugs without an FDA indication for management of insomnia, doxepin and amitryptaline are less commonly used for their sedating effect, in comparison to the other sedating antidepressants listed. Table 2.Summary of cognitive-behavioral therapy for insomnia components |
|
|||||||||||||||||||||||||||||||||||||||||||||