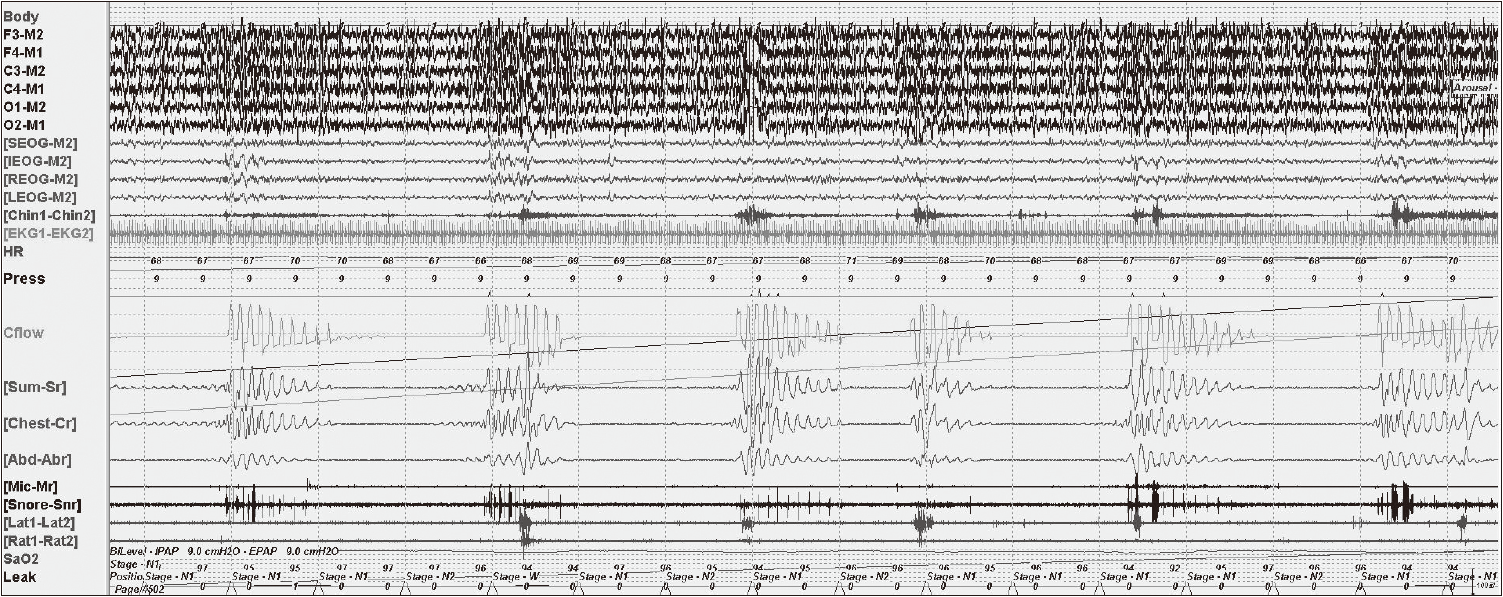
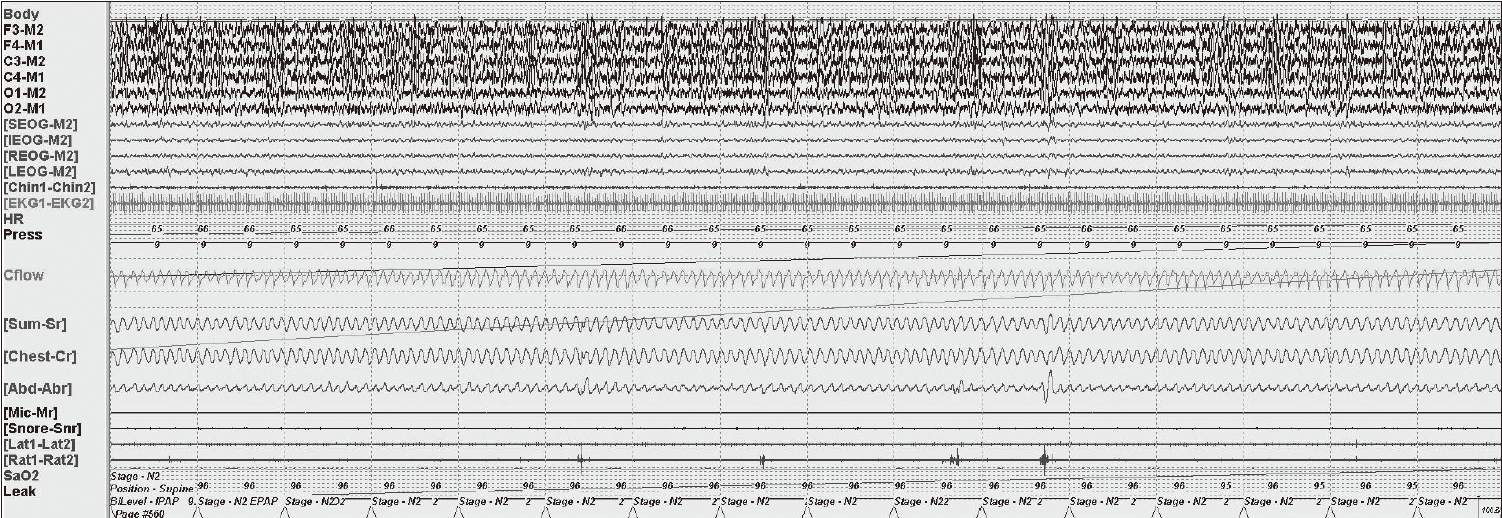
A 58-year-old man with end-stage renal disease on hemodialysis and hypertension presented with habitual snoring, observed apneas, and daytime sleepiness. His renal function remained stable during the course of evaluation and management of sleep apneas. The full-night diagnostic polysomnography (PSG) showed severe sleep apneas (apnea-hypopnea index 67.4). The main type of respiratory events is obstructive (obstructive apnea index 24.1) but central chemoreflex instability was also documented (central apnea index 2.9; mixed apnea index 3.5). On the diagnostic PSG, patient had no rapid eye movement (REM) sleep. So we could not document REM-related improvement or worsening of sleep-disordered breathing. We performed the first titration study one week after the diagnostic PSG, but patient did not tolerate continuous positive airway pressure (CPAP) and repetitively woke up (wake after sleep onset 50.9%; time in bed, 197.4 min) and only slept 94.5 minutes (sleep efficiency: 63.5%). The pressure was dialed up to 6.0 cm H2O but the apnea-hypopnea index was 10.2. The titration was considered unacceptable and patient did not accept CPAP therapy. As symptoms persisted, a second titration was performed two months later with zolpidem 10 mg at bed time. Sleep was successfully induced (Fig. 1). CPAP was titrated up to 9 cm H2O to normalize obstructive events and sleep fragmentations during supine REM sleep. Stable respiration and sleep was maintained after sleep onset until central sleep apneas abruptly emerged (Fig. 1). The time when central apneas emerged is about two and a half hours after sleep onset that coincided with the half life of zolpidem (1.5–2.4 hr).1 The pressure was titrated up to 10 cm H2O, but did not control respiratory events (apnea-hypopnea index 34.9; central apnea index 23.3), and sleep remained fragmented. Finally patient woke up and did not tolerate further titration (Fig. 1). The study was terminated at 3:36 AM (time in bed 246.0 min; total sleep time 233.0 min). At the second titration, CPAP at 9 cm H2O maintained airway patency during the stable sleep induced by zolpidem but central sleep apneas and periodic breathing emerged as the drug effect wore off (Figs. 1 and 2). Complex sleep apnea was diagnosed, and a third titration was performed to treat complex apnea with carbon dioxide modulation using enhanced expiratory rebreathing space (EERS).2 Central apneas and periodic breathings can be generated when the arterial carbon dioxide level falls below the apnea threshold.3 Therefore, preventing hypocapnia has a stabilizing effect on sleep-respiratory control. EERS was designed to provide a dead space-like effect using a non-vented mask and 4–6 inches of additional standard tubing.2,4 Three weeks after the second titration, the third study was performed with zolpidem 10 mg at bed time and with EERS. Between the second and third titration, CPAP had not been applied. Sleep was successfully induced and maintained with increased amount of slow wave sleep in the first half of the night. EERS of 50 mL was added from the beginning of the study and titrated up to 100 cc to minimize hypocapnia. As expected from the second titration, CPAP at 9 cm H2O and zolpidem successfully controlled sleep disordered breathing and sleep fragmentation in the first half night (Fig. 3). With CPAP, EERS and zolpidem, sleep was more consolidated with decreased arousals and increased amounts of slow wave sleep that was absent at the second titration. Three-and- a half hours after lights-out, the patient woke up for about 50 minutes, possibly from a zolpidem withdrawal effect (Fig. 3). Once the patient fell asleep again, CPAP at 9 cm H2O was implemented with EERS of 100 mL successfully prevented the emergence of central sleep apneas during the latter part of the titration (Figs. 3 and 4).
Emergence of central apneas with the possible withdrawal of sleep stabilizer due to a pharmacokinetic (half life) effect suggests that increased sleep-wake transitions is one of the contributing mechanisms of complex sleep apnea. We also documented the beneficial effect of EERS to control complex sleep apnea. Though the natural course and underlying mechanisms of complex sleep apneas remain to be fully determined, judicious use of hypnotics and EERS could aid in the management of many patients.5