Insomnia in Post-Hematopoietic Stem-Cell Transplant Patients in Jordan: Prevalence and Associated Factors
Article information
Abstract
Background and Objective
Insomnia is a common symptom that is experienced by the patients post hematopoietic stem cell transplant that interfere with recovery outcomes and patients’ quality of life. Little is known about insomnia among post hematopoietic stem cell transplant in Jordan and in other Arab countries. The purpose of the current study was to identify the levels of insomnia and the related factors in post hematopoietic stem cell transplant.
Methods
A descriptive cross-sectional correlational design was used to guide this study. Data was collected from 163 patients by the Arabic version of the Insomnia Severity Index (ISI).
Results
The participant’s average ISI was 14.06 ± 7.71 indicating sub-threshold insomnia. Regarding the insomnia levels, 23.9% of the participants reported no insomnia, 27.6% had subthreshold insomnia, 31.3% had moderate clinical insomnia, and 17.2% had severe clinical insomnia. A significant difference in insomnia levels in some related factors was reported including the higher educated patients (t = 2.40, p = 0.018), patients who received allogeneic transplants (t = -2.932, p = 0.004), and patients within a 30 days’ post-transplant (F (160, 2) = 61.03, p < 0.001).
Conclusions
In conclusion, the overall prevalence of insomnia among post HSCT patients was 48.5% (n = 79) that suggested clinical insomnia, and it was affected by several clinical variables. Further studies are needed to provide appropriate interventions to decrease insomnia levels among patients.
INTRODUCTION
The Center for Disease Control and Prevention defines insomnia as “an inability to initiate or maintain sleep. It may also take the form of early morning awakening in which the individual awakens several hours early and is unable to resume sleeping. Difficulty initiating or maintaining sleep may often manifest itself as excessive daytime sleepiness, which characteristically results in functional impairment throughout the day” [1].
It is common for patients after hematopoietic stem-cell transplant (HSCT) to have insomnia [2-4]. Cancer patients undertaking an HSCT procedure may be exposed to treatment protocols that include chemotherapy, which may induce multiple side effects, including insomnia [4,5]. It was reported that up to 43% of patients after HSCT with different cancer diagnoses suffered from insomnia. Furthermore, insomnia interfered with patients’ quality of life [6,7], impaired immune functions [8], caused memory problems [9], increased cancer-related fatigue [10], reduced survival [11], and may have implications for tumor progression [12].
Over the time of recovery, which may extend up to 100 days after HSCT, patients may complain of insomnia [13], which may be manifested as difficulty in maintaining sleep (n = 36, 82%), non-restorative sleep (n = 27, 61%), problems falling asleep (n = 23, 52%), difficulties falling back to sleep once awake (n = 21, 48%), and early morning awakening (n = 9, 21%) [3]. Previous studies emphasized that 77% of patients reported insomnia during hospitalization following HSCT [3]. On the day of transplantation, more than 30% reported insomnia [14]. This period is critical, because HSCT patients’ need more sleep in order to recover from illness [15].
Little is known about insomnia among cancer patients after HSCT in Jordan and other countries, largely because there have been no studies that used insomnia-specific measuring tools, such as ISI [16]. Most of the articles that examined sleep among HSCT recipients measured sleep with multi-items tools that were not constructed to measure insomnia and/or are difficult to score, such as the Pittsburgh Sleep Quality Index [4,17]. Hence there is a need to measure insomnia with a specific tool, such as ISI, to find fine details about the insomnia variables, which include the inability to initiate or maintain sleep, early morning awakening, difficulty initiating or maintaining sleep, and excessive daytime sleepiness, which may contribute to impairment in daily functioning [1].
Previous literature has identified many factors that are related to insomnia among patients after HSCT, such as socio-demographic variables, in addition to numerous clinical factors [18]. Age, gender, monthly income, educational level, work status, and marital status were among the strongest socio-demographic factors related to insomnia [13]. On the other hand, the clinical variables that have been reported in the literature as having a relationship with insomnia include therapy protocol, type of transplant, and time since transplant [18]. A study conducted by Jim et al. [18] showed that those who were younger (54.85 ± 12.43), unmarried (26%), or had allogeneic HSCT (46%) had more insomnia. Additionally, other researchers found that patients in the oldest age groups were the least likely to report insomnia (n = 28, 35.7%) [19]. Further, across all age groups, women reported more insomnia and tiredness. About 87% (n = 26) of women reported insomnia in allogeneic HSCT compared to 67% (n = 41) of men [4]. No previous studies have reported any significant relationship between income and educational level with insomnia scores, and this warrant further investigation.
There is a little attention paid to insomnia and its associated factors among HSCT patients [20]. Hacker et al. [21] showed that there are few studies that examined insomnia among HSCT patients or that explored the associated factors that affect insomnia. Thus our aim in this study was to identify the levels of insomnia and the related factors in post-HSCT patients.
METHODS
This study is descriptive and cross-sectional, and is aimed at assessing insomnia levels and related factors during the recovery period of post-HSCT patients, which may extend up to 100 days, in one of the biggest referral oncology hospitals, with a capacity of 352 beds, in Amman, Jordan.
Subjects
The participants in this study consisted of Jordanian cancer patients who had undergone HSCT. In order to evaluate the research questions, we used a G*Power (version 3.0.10; https://www.psychologie.hhu.de/arbeitsgruppen/allgemeine-psychologie-und-arbeitspsychologie/gpower) analysis to calculate the participants’ numbers [22]. In order to detect a significant difference in insomnia levels in patients’ demographic groups, assuming a medium effect size (Cohen’s d = 0.30), alpha = 0.05, power = 0.80, and using a two-tailed test, we found that a sample of 158 patients was needed. To allow for 15%–25% attrition, which may reduce the sample size and affect the study power, we recruited enough participants to have 200 subjects [23].
The inclusion criteria were HSCT patients, age above 18 years old, who can read and write in Arabic, and were in their first 100 days’ post-transplant. We excluded any patient with a known history of respiratory problems, such as sleep apnea, or cognitive impairments from the study.
Measures
We distributed a self-administered questionnaire to each participant by using an online SurveyMonkey. The package consisted of two parts; demographic and clinical characteristics sheet and the Arabic version of the ISI [24].
The Demographic and Clinical Characteristics Sheet
This sheet had all the questions about the demographic characteristics of the sample, such as age of the patients in years, gender (male/female), marital status (married/not married), educational levels (before or after high school), and monthly income in Jordanian dinars. We also obtained a few clinical features, such as diagnosis and time since HSCT, where the participants were asked to report how many days it had been since the HSTC, type of transplant (allogenic/autologous), and protocol of treatment regimen (chemotherapy alone, chemotherapy with radiation).
The Insomnia Severity Index (ISI)
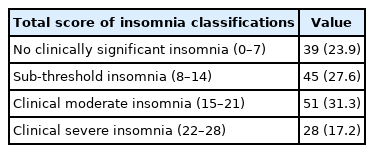
Morin et al. [25] designed the ISI to be a brief seven-item selfreported questionnaire to evaluate the severity of insomnia for the last 14 days. The ISI measures the symptom, the consequences, and the level of distress caused by the insomnia. The seven items ask about sleep onset, sleep maintenance, which includes nocturnal and early awakenings, sleep satisfaction, sleep interference with daily functioning, and distress caused by sleep problems [25]. Each item measures insomnia on a 5-point Likert scale ranging from 0 = no insomnia to 4 = severe insomnia. The scores of the seven items add up to a total score ranging from 0 to 28 [25]. A cut-off score for the total score was created by the original author as follows: no clinically significant insomnia (0–7), sub-threshold insomnia (8–14), moderate severity (15–21), and severe insomnia (22–28) [26].
The ISI demonstrated a high internal consistency of 0.88 [25], and an item to total significant correlation ranged from 0.32 to 0.71 [26]. Further, Bastien et al. [26] reported a significant convergent validity (r = 0.32–0.91, p < 0.05) of the ISI with the sleep diary. The Arabic version of the ISI demonstrated an excellent internal consistency (α = 0.84) among 35 healthy Arabic participants living in the USA [24].
Statistical Analysis
We analyzed data by using the Statistical Package for the Social Sciences version 23 (IBM SPSS Statistics for Windows, Version 23.0; IBM Corp., Armonk, NYm USA). We checked all data entered for outliers and missing data. We started data analysis by calculating the descriptive statistics for all variables, which included central tendency measures and measure of dispersion for all variables. Also, we obtained histograms for numerical variables and bar and pie charts for nominal variables. We obtained inferential statistics as appropriate, independent sample t-tests, analysis of variance (ANOVA) to detect any relationship between insomnia and numerical variables, and correlation coefficients to detect group differences in level of insomnia.
When we examined ISI in terms of demographic and clinical variables, as in previous studies, we treated numerical variables as categorical variables. We categorized age into four categories: < 24, 25–40, 41–60, and > 60. The participants’ income was divided into three categories: ≤ 400 JD, 401–600 JD, and > 600 JD. Also, we divided the time since transplant variable into three categories: 1–30, 31–60, and 61–100 days. We considered an alpha of 0.05 to be significant for all analyses.
Study procedure and data collection
We explained the aims and purposes of this study to the head nurses of the selected settings. The potential participants were inpatients and outpatients within 100 days after HSCT before the data collection started. On the day of data collection, the potential participants were invited to participate in the study. We approached them personally at the selected care settings and explained what the study’s aims and outcomes were. This study was approved by the Insitutional Review Board of King Hussein Cancer Center (IRB No. 20 KHCC 63). We uploaded a questionnaire package that included the demographic sheet questions and the Arabic version of the ISI as a SurveyMonkey and sent the link to the participants by WhatsApp messages. We contacted the participants by a follow-up phone call two days after recruitment to remind them to answer the questionnaires. We completed the data collection during the four months from May to August 2020.
RESULTS
In total, we distributed 200 questionnaires to patients. Only 163 patients (133 outpatients and 30 inpatients) completed the questionnaires, giving a response rate of 81.5%; 17 participants didn’t answer the survey, and 20 participants did not complete the survey.
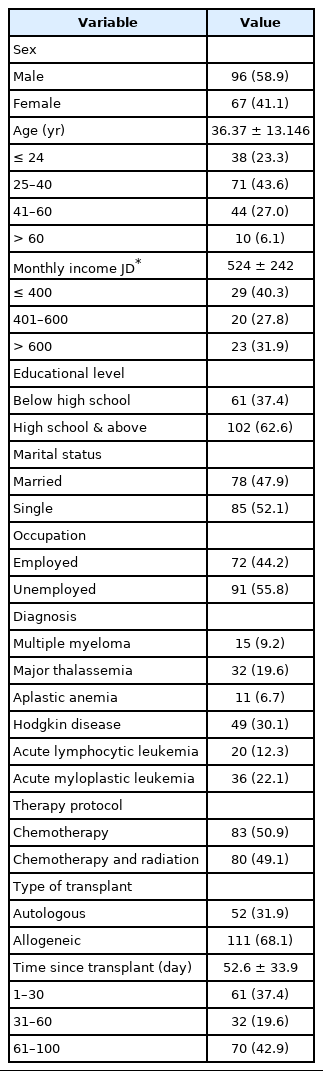
Table 1 shows the socio-demographic characteristics of the 163 (96 male and 67 female) participants. Most of the participants were less than 40 years old, with a mean of 36.37 ± 13.14. The mean monthly income of the participant was 524 ± 242 JD. More than half the participants (62.6%, n = 102) had received a high level of education. Further, about half the participants were single (52.1%, n = 85), unemployed (55.8%, n = 91).
Table 2 shows the clinical characteristics of the study sample. Most of the participants had Hodgkin’s disease (30.1%, n = 49); on the other hand, the lowest percentage of the participants (6.1%, n = 11) had aplastic anemia. In the treatment protocol, about half the participants had received chemotherapy (50.9%, n = 83). Most of the participants (n = 111, 68.1%) had an autologous transplant. The time since transplant was 5–99 days, with an average of 52.6 ± 33.9 days. Further, many of the participants were at 60 to 100 days post-transplant (42.9%, n = 70).
In this study, the total mean score of the ISI was 14.06 ± 7.71, which indicating that most of the sample had sub-threshold insomnia. We found that around half the participants (48.5%, n = 79) had moderate or severe insomnia. About 23.9% (n = 39) of the participants reported no insomnia, 27.6 % (n = 45) subthreshold insomnia, 31.3% (n = 51) clinical insomnia of moderate severity, which was the highest percentage of the total sample, and 17.2% (n = 28) severe clinical insomnia, which was the lowest percentage of the total sample; see Table 3. On average, participants needed less time falling sleep (1.86 ± 1.12), less difficulty in staying asleep (1.82 ± 1.12), and a lower rate of waking up too early (1.88 ± 1.19). On the other hand, the participants were not satisfied with their sleep (2.23 ± 1.24), felt that their sleep problem was noticeable to others (2.06 ± 1.25), worried about current sleep problems (2.02 ± 1.25), and felt that their sleep problems affected their daily functioning (2.23 ± 1.31) (Table 4).
In order to detect the relationship between insomnia and selected demographic variables, we explored the differences of insomnia scores in the different levels of demographic variables.
In the differences in ISI scores in demographic variables categories, an independent sample t-test indicated that patients with educations above high school (15.17 ± 7.35, n = 102) had significantly higher insomnia scores (t (161) = 2.40, p = 0.018). Also, the results indicated that patients with more than a high-school education had significantly more difficulty in staying asleep (1.96 ± 1.11), a higher rate of waking up too early (2.06 ± 1.15), were less satisfied with their sleep (2.38 ± 1.13), and felt more that their sleep problems affected their daily functioning (2.25 ± 1.17) (p ≤ 0.05). In contrast, patients after HSCT exhibited similar ISI scores regardless of age, gender, monthly income, marital status, or occupation (p > 0.05).
The independent sample t-test indicated that patients who received chemotherapy and radiation therapy (15.82 ± 7.59, n = 80) and who received allogeneic HSCT (15.18 ± 7.33, n = 111) had significantly higher insomnia scores [t (161) = -2.932, p = 0.004 and t (161) = -2.760, p = 0.006, respectively]. Furthermore, we did a one-way between-subjects ANOVA) to compare the effect of time after transplant on ISI total score for 1–30, 31–60, and > 60 days. There was a significant effect of time after transplant on ISI total score at the p < 0.05 level for all three categories of time [F (160, 2) = 61.03, p < 0.001]. Post hoc comparisons using the Tukey honestly significant difference test indicated that a significantly higher mean ISI score was reported by patients in the 1–30 days category (19.62 ± 7.00). Further analysis showed a negative correlation between increased number of days since transplant and total ISI score, which was lowest after 61 days or more (r = 0.714, p < 0.001).
Additionally, we found that patients at day 60 post-transplant had significantly less difficulty in staying asleep (1.10 ± 0.92), less difficulty in falling asleep (1.07 ± 0.80), less waking up too early (1.16 ± 0.94), and more satisfaction with their sleep (1.37 ± 0.97), and felt less that their sleep problem affected their daily functioning (1.26 ± 1.00), felt that their sleep problem were less noticeable to others (1.14 ± 0.94), and felt less worried about current sleep problems (1.37 ± 1.08) (p < 0.001).
DISCUSSION
In this study, we found that most HSCT patients presented with various degrees of insomnia (sub-threshold, moderate, or severe), but a lower percentage of our patients had no clinically significant insomnia. This finding is consistent with that of previous studies, several of which stated that insomnia is the most commonly reported sleep problem among HSCT patients posttransplant [4,19,27,28]. For instance, according to Boonstra et al. [4], most HSCT patients had some degree of insomnia (48% sub-threshold, 23% moderate, 3% severe), but 26% of them had no clinically significant insomnia. Also, similar results were reported by Jarvis et al. [27], where 42.2% of HSCT patients had sub-threshold insomnia, 30.3% had moderate insomnia, and 27.3% had no significant insomnia. Faulhaber et al. [19] reported that 23% of HSCT recipients complained of insomnia as the main sleep disorder one to ten years after HSCT treatment.
Moderate insomnia might be experienced by patients after HSCT for several reasons, such as the lengthy hospitalization, multiple medications and fluids, environmental influences [4], the effects of conditioning therapy, immunosuppression, stress, and adverse physical side effects of the intensive therapeutic regimen [29], and the side effects of the conditioning regimen.
We found that patients after HSCT exhibited similar ISI scores regardless of age, gender, monthly income, marital status, or occupation. Similar results were reported by other studies [4,13,30]. In contrast, Hacker et al. [21] reported a significant relationship between age and insomnia among HSCT patients. They found that younger patients reported more severe insomnia than did older patients [21], perhaps because of the subjectivity of the self-reported assessment of insomnia. They suggested that elderly patients might have experienced chronic insomnia before HSCT, which may have interfered with their judgment of the changes during hospitalization, whereas younger patients may have experienced new onsets of insomnia, therefore eliciting more pronounced responses.
In sex, our results were consistent with other studies that examined sleep among both genders post-transplant [31,32]. In the general population, insomnia among females was higher than in males; hormonal changes during the menstrual cycle, pregnancy, and post-menopause were the main explanations for this difference in insomnia level [33]. The difference between our results and those for the general population may arise because a female patient who undergoes HSCT may receive oral contraceptive medication (such as Yasmin and Provera) that interferes with her normal hormone levels and menstrual cycle; consequently, she experience insomnia much as male patients do.
We found a statistically significant relationship in insomnia scores between HSCT patients with different educational levels, which no other study has found. However, our results can be explained by the nature of educated patients, who may overthink the pros and cons of stem-cell transplantation, consume time searching multiple sources on the internet to find information about every issue about the transplant procedure, the side effects of chemotherapy, and consequences and side effects after HSCT.
We found that insomnia was significantly associated with therapy protocol, type of transplant, and time since transplant, and found a significant difference with therapy protocol among HSCT patients in total ISI score. This preliminary evidence for the role of therapy protocol on insomnia post-HSCT has not been reported by previous studies. These results might arise from the side effects of radiation therapy, including sleep problems [34]. Radiation therapy causes asymptomatic injury to normal tissues surrounding the tumor (which leads to the expression of proinflammatory cytokines (interleukin-6 and tumor necrosis factor-α). These proinflammatory cytokines are significantly correlated with sleep disturbances and sleep quality [35].
Furthermore, our result agrees with the findings by Miaskowski and Lee [36], who monitored sleep using wrist actigraphy for 24 patients receiving radiation therapy for bone metastasis. They found that 75% of the patients had bad sleep efficiency. The most common reasons for awakening were for urination or pain [36]. Additionally, Hickok et al. [34] conducted a study among 1229 cancer patients receiving radiotherapy; 51% of them reported that they had sleep problems, perhaps because of the association between fatigue, drowsiness, and difficulty in sleeping. Also, Thomas et al. [37] found that prostate-cancer patients receiving radiation therapy had sleep problems during or after treatment; there was a significant negative correlation between the period of the course of treatment and sleeping hours.
We found that patients who had received allogenic transplants had statistically higher ISI scores than did autologous recipients. Our result agrees with Rischer et al. [3], who found that sleep quality differs between autologous and allogeneic transplant patients, because allogeneic patients require more time to recover from treatments as well as earlier discharge from a hospital than do autologous patients. Also, conditioning, which was used only for allogeneic patients (busulfan and cyclophosphamide), was a risk factor for insomnia after HSCT [19].
Furthermore, a significant difference in ISI total score was displayed between several categories of time since transplant. The link between sleep disorders and days post-transplant was reported in several studies; a negative trend was clear with ISI total score and time since transplant [13,18,38]. Our data confirm the findings of Rischer et al. [3], in which the prevalence of sleep disturbances among patients receiving HSCT decreased from 77.3% during the hospital stay to 28.1% 100 days post-transplantation. Similarly, Bevans et al. [14] reported that the prevalence of insomnia decreased from day 0 to day 100. The prevalence of insomnia gradually reduced from 88% at day 0, 65% at day 30, and 53% at day 100. The decrease of insomnia was explained by the improvement in the patient’s physical function and transition from the hospital to the home that reduces psychosocial symptoms [14].
Limitations of the study
Definitely, this study is not without limitations; the following are its possible limitations. We conducted the study in a single setting with minimal differences in the management of patients in the different clinical setting; so the data could not be generalized among all Jordanians. Another possible limitation is that data collection was implemented by a non-probability convenience sample. The sample consisted of patients who were willing to participate in the study; hence patients who did not choose to participate may have differed from those who did participate. The voluntary sampling method may limit the generalizability of the findings. Also, self-reporting is considered to be subjective data, and patients may have profounding responses. We did not assess the important role of medication, comorbidity, immunosuppression, laboratory findings, or metastasis on insomnia, nor did we control the effect of these variables by multivariate analysis; so we encourage future research to evaluate how these important factors affect insomnia among patients after HSCT. Also, future researchers may be encouraged to conduct interventional studies using behavioral therapies to reduce insomnia in patients after HSTC. Therefore, surveying sleep disturbances can be an integral part of routine HSCT follow-ups, and its effect should be investigated further in future prospective studies.
Conclusion
We investigated the levels of insomnia and their relationships with demographic and clinical variables in post-HSCT patients, in whom the overall levels of insomnia was 48.5% (n = 79), which suggested clinical insomnia. We also found a significant relationship between ISI score and demographic variables, such as education level. Further, we found a significant relationship between ISI score and clinical variables, such as the protocol of therapy, type of transplantation, and time since transplant. It would be meaningful to study the factors that predict the prevalence of insomnia and the effect on insomnia of other factors, such as nonpharmacological interventions, including sleep hygiene measures, restricting caffeine intake, participating in physical activity, such as walking, reducing fluid intake two to three hours before bed, and setting a sleep schedule.
Notes
Availability of Data and Material
The datasets generated or analyzed during the study are available from the corresponding author on reasonable request.
Authors’ Contribution
Conceptualization: Abdalrahman O. Data curation: Abdalrahman O. Formal analysis: Suleiman K. Investigation: Abdalrahman O. Methodology: Suleiman K. Project administration: Abdalrahman O. Resources: Suleiman K. Software: Suleiman K. Supervision: Suleiman K. Validation: Abdalrahman O. Visualization: Abdalrahman O. Writing—original draft: Abdalrahman O. Writing—review & editing: Suleiman K.
Conflicts of Interest
The authors have no potential conflicts of interest to disclose.
Funding Statement
None.